
What is Sudden Unexpected Infant Death (SUID)?
According to the Centers for Disease Control and Prevention ([CDC], 2018), sudden unexpected infant deaths (SUID) refers to:
- Sudden infant death syndrome (SIDS)
- Accidental suffocation and strangulation in bed
- Other unknown causes during the first 12 months of life
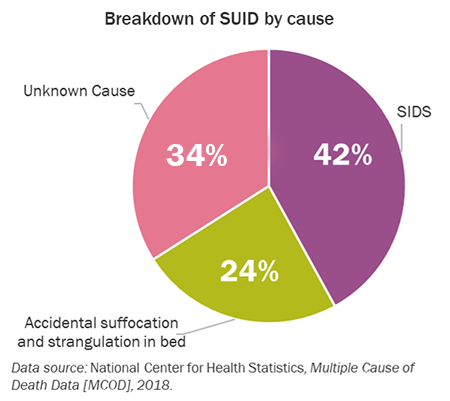
Each year in the United States, approximately 3,500 infants die suddenly and unexpectedly. The frightening fact about SUID is that it can happen without warning and to infants who seem otherwise healthy.
In 2016, there were about 1,500 (42%) deaths due to SIDS; 1,200 (34%) deaths due to unknown causes; and about 900 (24%) deaths due to accidental suffocation and strangulation in bed. The pie chart shows the breakdown of SUID by cause.
Racial/Ethnic Differences in SUID
SUID rates per 100,000 live births in American Indian/Alaska Native (AI/AN) and black infants are more than twice those of white, Hispanic and Asian/Pacific Islander (A/PI) infants. The graph below illustrates racial/ethnic differences in SUID rates.
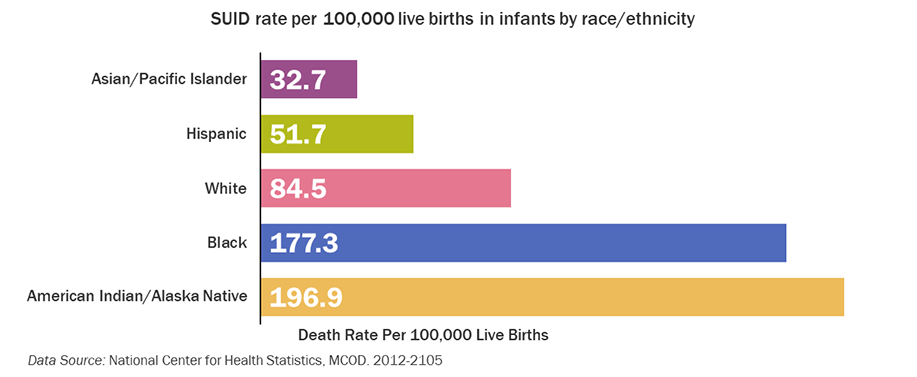
Risk Factors for SUID
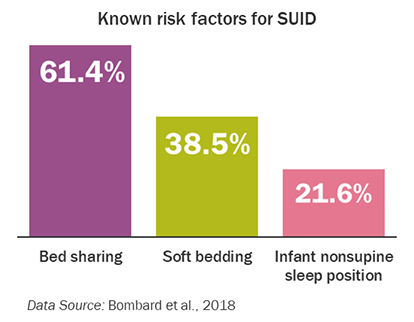
Although it is not fully understood why infants die suddenly and unexpectedly, several factors have been attributed to suffocation and strangulation in bed due to unsafe sleeping conditions. Infants sleeping on their stomachs, use of soft bedding (e.g., blankets, pillows, and bumper pads), bed sharing, exposure to smoking, caregiver alcohol use, and caregiver drug use are risk factors for SUID (Moon, 2016; Moon, Hauck, & Colson, 2016).
A study based on the CDC surveillance project called PRAMS, the Pregnancy Risk Assessment Monitoring System (Bombard et al., 2018), found:
- More than 1 in 5 mothers with a recent live birth placed their infant in a nonsupine sleep position (on side or stomach)
- More than 1 in 3 mothers used at least one type of soft bedding
- Nearly 2 in 3 mothers reported bed sharing with their infant
Unsafe sleep practices are higher among mothers in minority racial/ethnic groups, younger than 25 years of age, and with less than or equal to 12 years of education, suggesting that clear and culturally appropriate interventions are needed to reach these populations.
A recent study using the 2004 to 2014 data from the National Center for Fatality Review and Prevention Child Death Review Case Reporting System found that 13.1% of infant sleep-related deaths occurred under non-parental supervision (Lagon, Moon, & Colvin, 2018). Infants who died during non-parental supervision were placed in unsafe sleep positions, such as on their stomachs, or in unsafe locations, such as couches. These findings underscore the importance of educating all caretakers – babysitters, relatives, and friends – on known risk factors.
Resources on Reducing SUID and Promoting Safe Sleep
The American Academy of Pediatrics recommends the following practices to reduce SUID risk (Moon, 2016):
- Supine (on back) sleep position
- Firm sleep surface
- Room sharing without co-sleeping or bed sharing
- Sleep environment free of objects
- Avoidance of pre and postnatal exposure to tobacco smoke
Another resource is the Safe to Sleep campaign (formerly known as the Back to Sleep campaign), a collaboration between the CDC and National Institute of Child Health and Human Development (NICHD). The campaign provides education and strategies to reduce SUID to caregivers, health care providers, and others. Information and educational materials about sharing safe sleep messages and reducing SUID are available on NICHD’s website.
With the rates higher in minority populations, especially American Indian/Alaskan Natives and blacks, there is a need to address SUID disparities. Providing culturally-sensitive education and interventions are necessary steps to reduce SUID in high-risk populations. The National Institute for Children’s Health Quality proposes strategies to address these disparities in their webinar “Improving Safe Sleep Conversations: Strategies for Helping Families Adopt Safe Sleep Habits.” These strategies include engaging fathers and other infant caregivers in infant care discussions in a non-confrontational manner, utilizing home visiting services to observe infant sleep practices, and finding new opportunities and settings to discuss safe sleep (e.g., Women, Infants, and Children offices).
The Children’s Safety Network (CSN) has additional resources available on SUID, including a recorded webinar: “Safe Infant Sleep: Innovative National and State Efforts to Protect Our Youngest.”
References
Bombard, J. M., Kortsmit, K., Warner, L., Shapiro-Mendoza, C. K., Cox, S., Kroelinger, C. D., … Barfield, W. D. (2018). Vital signs: Trends and disparities in infant safe sleep practices — United States, 2009–2015. Morbidity and Mortality Weekly Report, 67(1), 39-46.
Centers for Disease Control and Prevention. (2018). Sudden unexpected infant death and sudden infant death syndrome. Retrieved from https://www.cdc.gov/sids/data.htm
Moon, R. Y. (2016). Task Force on Sudden Infant Death Syndrome, SIDS and other sleep-related infant deaths: Evidence base for 2016 updated recommendations for a safe infant sleeping environment. Pediatrics, 138, e20162940.
Moon, R. Y., Hauck, F. R., & Colson, E. R. (2016). Safe infant sleep interventions: What is the evidence for successful behavior change? Current Pediatric Review, 12(1), 67-75.
National Center for Health Statistics. (2018). Multiple Cause of Death Mortality Data. Hyattsville, MD.